Tonsillitis
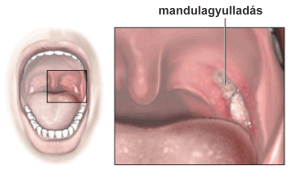 Tonsillitis usually starts with high fever, especially in children (sometimes accompanied by chills).
Tonsillitis usually starts with high fever, especially in children (sometimes accompanied by chills).
Indisposition is typical. A burning sensation and pain occur in the pharynx, most pronouncedly when swallowing.
Pain may radiate to the ears.
Breath is fetid, while the tongue is coated.
 Lymphatic nodes on both sides of the neck and at the angle of the jaw are swollen and painful to the touch.
Lymphatic nodes on both sides of the neck and at the angle of the jaw are swollen and painful to the touch.
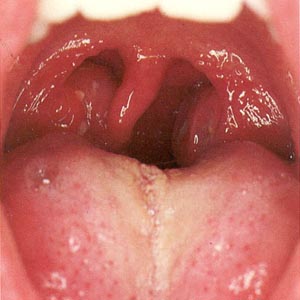
Both tonsils are typically swollen and injected, and the mucosa of the pharynx is sanguine.
Palatine tonsils, the pharynx, and pymphatic tissues are coated with yellowish and often follicular fur.
When pressed, tonsils emit a thick and fragmented detritus.
Causes
 Tonsillitis is usually caused by beta-hemolytic streptococcuses, sometimes by straphylococcuses, pneumococcuses or a mixed flora, and rarely by Haemophilus influenzae, the Coli-bacterium, viral infection.
Tonsillitis is usually caused by beta-hemolytic streptococcuses, sometimes by straphylococcuses, pneumococcuses or a mixed flora, and rarely by Haemophilus influenzae, the Coli-bacterium, viral infection.
The oral cavity and the pharynx always contains bacteria.
Such “physiological” germs include saprophytes, streptococcuses, pneumococcuses, fusobacteria, Neisseria, lactobacteria, staphylococcuses, etc.
If their environment changes, these “domestic” germs can become pathogenic even for the same individual’s body.
A viral infection can prepare the way for bacterial superinfection, including for tonsillitis.
Diagnosis
 Hystopathologically, abscesses containing inflamed cells form in the tonsils and a fibrinous fur forms on its surface.
Hystopathologically, abscesses containing inflamed cells form in the tonsils and a fibrinous fur forms on its surface.
The symptoms lend themselves to diagnosis easily: an acute flare-up with (high) fever, typically with sore throat and difficulty swallowing.
Laboratory results: blood work indicative of inflammation, an increase in white blood cell count, gradual decrease.
A general examination is necessary, including examination of heart and circulation and urine analysis.
I n cases suspected of diphtheria, vaccination is strongly recommended.
n cases suspected of diphtheria, vaccination is strongly recommended.
In case of suspicion of mononucleosis, blood work and serological tests are necessary.
Other forms of angina (such as scarlet fever, diphtheria, infectious mononucleosis, Pfeiffer’s disease, agranulocytosis, leukemia, tonsil hyperkeratosis, and secondary syphilis) should be treated separately from tonsillitis.
In the case of unilateral occurrence of tonsillitis, peritonsillar infiltration or abscesses, tuberculosis, or tonsillar tumor are possible.
Treatment
 Bed rest is important. Inducing perspiration is important at the outset.
Bed rest is important. Inducing perspiration is important at the outset.
Treatment of pain and fever. Liquid and pulpy diet.
Penicillin in big doses for 8 days (in order to prevent accompanying and consecutive complications).
No local antibiotic is recommended.
Oral and dental hygiene is to be maintained: oral disinfection, pharyngeal gargling, and, if necessary, pain medication are to be applied.
Compress on the neck is also recommended.
Course
 Inflammation is usually cured within a week.
Inflammation is usually cured within a week.
Accompanying or consecutive complications sometimes develop, such as laryngeal edema, difficulty breathing, otitis, maxillary sinusitis.
Unfortunately, sometimes complications such as rheumatic fever can also develop, often occurring after an asymptomatic interval of 4-6 weeks.
Myocarditis, pericarditis and acute nephritis can sometimes occur.
In order to prevent these, repeated urine analysis is recommended after recovery from tonsillitis.
In case of follicular tonsillitis, the most important recommendations are vaccination (to exclude diphtheria), urine analysis (to exclude kidney diseases), and quantitative blood work (to exclude mononucleosis).
Hits: 9753





